Strive not to be a success, but rather to be of value.
– Albert Einstein
Hi. My name is Mike, and I’m recovering from plantar fasciitis.
Check that – I’ve recovered from plantar fasciitis.
Na na NA na, hey hey hey, good-bye…
Plantar fasciitis accounts for roughly 10% of all running injuries. And yet judging by the sheer number of stories I’ve heard from runner friends in recent months – maybe because PF creates such lasting memories – 10% feels awfully conservative. I’ve heard stories from all directions – on email, on Facebook, from our CPA’s husband, while shopping for running shoes at REI, and while standing in line to use the pre-race porta-potty at the Big Sur International Marathon (and the lines weren’t even that long).
Collectively these stories would read like one of the “Choose Your Own Adventure” books I loved as a kid – some stories ended happily, with the PF dragon vanquished through either specific or vague treatments; other stories ended less auspiciously for those still struggling with chronic heel pain. And in at least one case the dragon won the day, flaming breath scorching its discouraged prey to the extent that he hung up his running shoes for good.
But after three consecutive 60+ mile running weeks, I’m ready to call my own Operation: Heal Heel a resounding success. And if you’re struggling with plantar fasciitis, then hopefully the next 2,000 words (and three short videos) will be of value in helping relief roll down like waters, and recovery like a mighty stream.
Knowing PF now as I do, I’d like nothing more than for my experience to help someone else recover quickly and completely. As a runner and a biologist, I think about injuries and developmental biology in the same way – I can’t truly appreciate how something works, until I understand what happens when it doesn’t. I now have a better understanding of why – in my case, at least – PF happens.
So I want to share the treatment plan that relieved my plantar fasciitis and enabled my return to running in less than a month – not with some heel pain, not with less heel pain, but with no heel pain.
We’re constantly urged to strengthen our core, or stretch our hamstrings, or mobilize our glutes, or engage our hip flexors. But aside from “foam roll your calves,” much less attention is paid to what goes on between the knees and ankles. Thing is, the knee bone really is connected to the ankle bone, so ignore the inner workings of the lower leg at your own risk. For me, plantar fasciitis exposed the widening (yet reparable) gap between the “calves” and the “calve-nots”.
Even if you don’t have PF but feel like your stride is just inexplicably off, this may be a good place to start – before you focus too much time and effort on trying to figure out what it means to “mobilize” one’s glutes.
What didn’t work
First, an important cataloging of the pre-Big Sur approaches that had little to no effect on the progression or severity of my PF. I pursued each of these at various times, while reducing my weekly mileage dramatically in an effort to have my cake (healing) and eat it too (training):
1) Rest – During a two-week stretch in March, when I should have been ramping up for Big Sur, I ran only one day. As a runner, nothing is more frustrating than resting an injury without a well-defined plan of attack – watching helplessly as the days and weeks creep by, relying on faith and positivity to heal you while assuming that recovery is just a matter of time. Turns out faith and positivity are no match for plantar fasciitis… two weeks on the shelf (in combination with options 2-7 below) did nothing to improve my injured heel. And so, not wanting to embarrass myself (or worse, DNS) at Big Sur, I returned to training while promising myself I’d take time off to fully recover – after the race.
2) Frequent icing – This publication and this video might explain why ice did nothing more than numb the pain in my heel.
3) Ibuprofen – Granted I wasn’t popping them like breath mints as some runners do, but my brief foray into “Vitamin I” offered no discernible relief.
4) Vigorous massage – Much like other forms of massage, Active Release Techniques on both calf and heel offered exquisite though short-lived relief from the pain.
5) Hokas – I tried both the Stinson Tarmac and Conquest models for a couple of weeks each. Thanks to their odd geometry and narrow toe box, I was able to relive the thrill of ultrarunning at non-ultra distances, since both models quickly chafed and blistered my feet in places I’ve never had blisters before (the underside of my big toe? really?). More importantly, they did nothing to relieve my PF.
6) Orthotics – I have custom orthotics from several years ago that I no longer wear, so in the interest of improved arch support, I dusted them off and slid them into my running shoes. I was rewarded with curious new aches and pains that competed with the heel pain rather than replacing it. Like flipping a switch, no more orthotics meant no more new aches. Unfortunately, my heel pain persisted.
7) Taping – Wrapping my foot in either standard athletic tape or kinesiology tape (‘cuz I liked the name, “KT Tape”) helped to some degree, but who wants to walk around with a taped foot 24 hours a day? Besides, the positive effect quickly subsided when I realized my podiatrist charged – or at least tried to charge – $48 just to tape my foot. Presumably the tape he uses is interlaced with gold fibers excavated from the ceremonial robes of dead baby pharaohs.
Enter PT (i.e. What did work)
In the midst of my PF-addled and Internet-accentuated confusion, my best decision turned out to be my choice of podiatrist. Not because the fellow I chose relieved my heel pain himself – he didn’t – but because he referred me to Doris.
Doris showed up at our front door on a Friday afternoon in early May, with her padded torture table tucked under her arm. But no, we weren’t filming Pulp Fiction 2 – Doris is a physical therapist who works extensively with NBA players, including the L.A. Clippers. Her intimate familiarity with sports injuries became immediately apparent, as within minutes she’d identified (without any prompting from me) two hypersensitive trigger points in my lower leg – muscle sorenesses I’d largely been ignoring for some time, filing them as so many runners do under “running niggles that will eventually work themselves out”.
As she worked diligently to remove the bullet I swear was lodged in my lower leg, it suddenly hit me, in a moment of pain-evoked clarity, that my heel was the least of my problems.
Because through all of her manipulations, Doris ignored my heel – didn’t poke it, didn’t prod it, didn’t invoke Reiki Crystal Healing to re-align its shakra (we are in L.A., after all). Hadn’t she heard me say “plantar fasciitis”? Sure I’d love to have stronger calves, but maybe later, after this PF demon was exorcised…
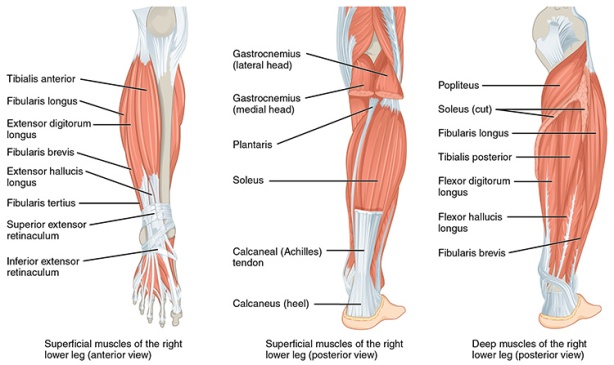
Source: OpenStax CNX at Rice University
Instead, she explained (without any overt reference to the heel) that I’d developed imbalances in my lower leg and that I needed to strengthen the offending muscle groups, among them the peroneus brevis, peroneus longus, tibialis anterior and extensor digitorum longus. And she prescribed three simple exercises that would ultimately become my holy trinity of PF relief. I’ve included brief video demonstrations below… for the first two you’ll need a Thera-Band (the color of the band determines its resistance; I’ve been using high-resistance black).
My PF affected the main (aponeurosis) and lateral (outer) plantar fascia… if your pain extends to the medial (inner) plantar fascia, you’ll want to consider similar exercises that target the medial calf muscles as well.
Perform each exercise twice daily. It’s that easy. No really, it is.
1) While sitting in a chair, strap the Thera-Band around your injured foot as shown. Using your knee as a fulcrum, evert (i.e. rotate your foot outward) the injured foot away from the healthy foot. Be sure to rotate only your foot – don’t twist your leg. Return to original position and repeat until the muscles in your lower leg start to burn, then hold in the fully everted position for 20-30 seconds, and finish with 20-30 more:
2) Tie the Thera-Band around something stable (e.g. a bannister rail, table leg or fat sleeping kitty) and, while sitting on the floor, strap it over your forefoot as shown. Straighten your leg until the band is taut. Keeping your heel in place, flex your toes and forefoot toward your body against the band’s resistance. Return to original position and repeat until the muscles in your lower leg start to burn (in the video you can see my anterior tibialis – the targeted muscle in this exercise – flex with each movement). Then hold your foot in the flexed-forward position for 20-30 seconds, and finish with 20-30 more:
3) Eccentric calf stretches: I know the name of this one, since it’s a common treatment for Achilles tendinopathy. Stand with both feet on a raised step (a staircase or curb will work) and balance yourself with one hand on a wall or tree. Raise yourself up on the toes of both feet, then lower yourself back down slowly and support yourself on only your affected foot, so that your heel dips slightly below parallel with the step. Hold this pose for 2-3 seconds, then return to original position and repeat 15-20 times:
Doris offered that I could cautiously return to running after a week, but by that point I was once bitten, twice shy. Wary of another false start, I waited patiently until I could dig my thumb into my heel without significant pain, gave myself a bonus week of rest for good measure, and then mixed in three days of rugged hiking out in Sequoia & Kings Canyon National Parks.
During this time I also slept with a PF night splint on my foot every night, not always the most comfortable proposition but definitely one of the few nuggets of conventional PF wisdom that helped. The fellow I met in the porta-potty line at Big Sur still struggled with his PF – he’d worn the night splint for a while but admitted to stopping because, in his words, “It kind of kills the mood, you know?” Considering that both Katie and I are in a far better mood when I’m able to run – no, I don’t know. And the splint pops on and off in seconds.
Exit PF
Exactly four weeks after my session with Doris, I was running two pain-free miles on the West L.A. College track. The next day it was three, and then four, and then – on my fourth visit to the track in five days – I managed a very gentle five miles, as every tendon and ligament in my legs revolted. And yet despite my reflexive hesitation, the foot felt springy and strong, like a brand-new body part I’d just pulled out of an Amazon box, with its odometer set to zero and “new heel smell” still intact.
I’d never been so happy – so absurdly, unapologetically happy – to run on the track before. Pharrell Williams had nothin’ on me. And to be able to hop out of bed each morning now without pain, or bound off a curb and land on my formerly stricken foot, just feels – WOW. Hopefully I’ll never take either sensation for granted again… but then again, I hope I do.
I’ve ramped up my mileage fairly quickly, running five days and cross-training two days per week, and still do my Thera-Band exercises two or three times a week (more often for the eccentric calf stretches). I feel occasional soreness on the lateral side of that foot, though not in the heel, and it almost always dissipates by the next morning. And I’ve taken to wearing my orthotics in my slippers, to provide more support on our hardwood floors.
But I don’t ice my foot, I don’t take ibuprofen, I run the vast majority of my miles on concrete (since trails here are less easily accessible than in Berkeley), and my foot feels comfortable in maximally cushioned Altras, moderately cushioned Sauconys or minimally cushioned Merrells. The cherry on top of this recovery sundae is that my stride feels more fluid and balanced than it has since I-can’t-recall-when.
And we’ve finalized our plans for Berlin in September.
I’m not entirely sure what caused my plantar fasciitis in the first place, and so I’m hyper-aware that it could return. At the same time I’m ever-vigilant of the need to keep my calf muscles strong and limber. I can’t necessarily say weakness in my calf muscles caused my PF, but I can say with certainty that strengthening them relieved it. Hopefully my experience can help runners and non-runners alike reach a similarly happy ending, without the frustration of first drifting among various pseudo-treatments that target the symptom while ignoring the cause.
So if you’re currently sidelined with PF, or have a PFrustrated PFriend, it can’t hurt to give these exercises a shot or pass them along. Certainly not as much as your heel hurts now. Besides, there’s always room for another voice in the Chorus of The Cured… one, more, TIME!
Na na NA na, hey hey hey, good-bye…
In the meantime, anyone in the market for a (gently used) night splint should drop me a line… though I’d hate to be responsible for killing your mood.
If you’re battling plantar fasciitis or other running injuries, feel free to contact Doris Martel at: dorismartel AT gmail DOT com. My one-hour appointment was ultimately worth a whole lot more than what I paid.
UPDATE (4 Aug): Julie (who recently entertained her own PF goblins) astutely brings it to my attention that this post’s title may be a bit misleading given that, well, I’m also a doctor. But since PhDs are real doctors and you should consult one whenever possible, and since it’s my blog, I’m willing (as always) to make an exception for myself.









